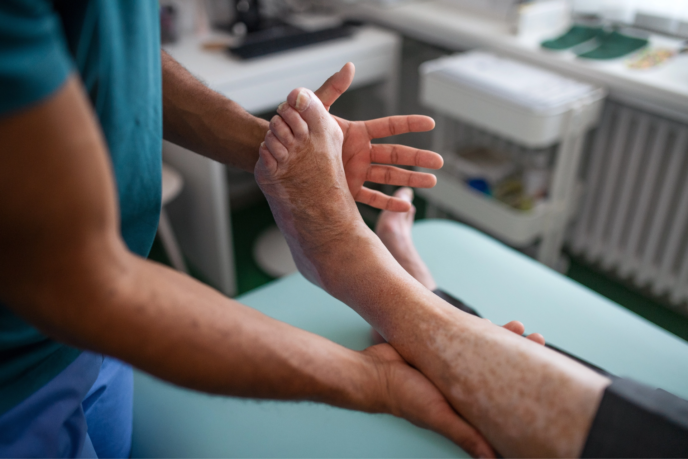
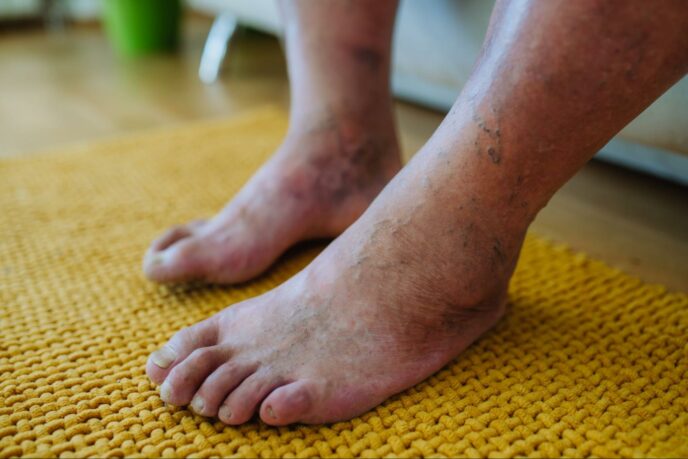
Risk Factors of Foot Ulcers in Diabetics
Dr. Chris Donikyan is board certified in Diagnostic Radiology, with a certificate of added qualification in Vascular and Interventional Radiology. Dr. Donikyan has years of experience treating diabetic patients with peripheral artery disease and non-healing wounds. In this blog interview, Dr. Donikyan explains the risk factors of foot ulcers in diabetics.
How Common is it for Diabetics to Develop Foot Ulcers?
It’s very common for diabetics to develop foot ulcers. It’s estimated that at least 15 to 20% of diabetics will at some point develop those types of ulcers. This is especially true for people who have poorly controlled blood sugar. The blood flow to their feet is compromised.
A normal blister that might develop from a small trauma, banging your foot against a chair, or just being on your feet all day (that normally would heal), won’t heal in a diabetic because the blood flow is compromised.
In order to heal wounds, you need blood flow. If there is arterial disease involving the small arteries that branch out into your toes and the bottom of your feet, compromised blood flow is going to make it so that those wounds won’t heal. It’s very important that diabetics stay on top of hygiene and diligent wound care.
What are the Risks and Consequences of Diabetics Not Treating Foot Ulcers?
Potentially, a foot ulcer that ultimately blossoms into a huge ulcer and then compromises even the bones of the feet will turn into a downward spiraling cascade of events. A wound can turn into a bone infection, which can, in turn, lead to amputation of digits. From there, it’s just a very difficult thing for a diabetic to deal with, losing toes, a foot, or a limb. These can be prevented just from being aggressive with wound care and being aggressive with controlling blood sugar.
It’s all about prevention. So, if we can stay on top of what the arteries look like, what the skin looks like and be proactive instead of reactive, I think that’s the most important thing.
Why Do Patients with Peripheral Artery Disease (PAD) Present with Painful, Non-Healing Ulcers in the Distal Foot and Toes?
Patients with PAD have developed calcium and plaque in their arteries, just the same way you can get arterial disease in your heart. You can get it anywhere in your body.
If you take people who have high cholesterol and high blood pressure and add to that diabetes, it’s a recipe for creating plaque that is going to compromise the blood flow to the digits — to your feet and your toes. Because the blood flow is limited or it’s decreased, wounds can’t heal. That’s why these ulcers develop and become a very bad source of infection.
Why Do Diabetics Have an Increased Risk of Developing PAD?
It’s a function of controlling their sugar and their glucose levels. Unfortunately, it’s not usually just diabetes that affects these patients. They have problems that people without diabetes have. They have high blood pressure, increased cholesterol, and triglycerides among other things. They can be overweight, obese, or sedentary in their lifestyle. Add to that diabetes and it just compounds everything. It accentuates the disease process, the building up of plaque. Unfortunately, for diabetics, everything gets accelerated. Everything increases tenfold in terms of developing plaque and arterial disease.
What are the Treatment Options for PAD and People with Diabetes?
Number one — and again, it’s a proactive mentality — do surveillance of the arteries in your limbs, your neck, your carotid arteries. We need to do screenings to make sure that everything is open. Annual well visits help us ensure that the blood flow to all those parts of your body is adequate, if not optimized.
Once we detect something that could be a problem, there are non-invasive ways to image it with ultrasounds, CT scans, and things like that. Angiography, ballooning, and stent placement helps us prevent having to go into the O.R. and do major surgery and bypasses.
The more that we are proactive in surveillance and trying to minimize what needs to be done, the better it is and the more long-lasting the results will be.
Request an Appointment with Dr. Donikyan
Request an Appointment today with Dr. Donikyan at Fishkill Endovascular if you are at risk for diabetic foot ulcers, or request an appointment at your nearest American Endovascular center today!
Related Blogs & Videos
Learn more about vascular health, prevention, and care for Peripheral Artery Disease.