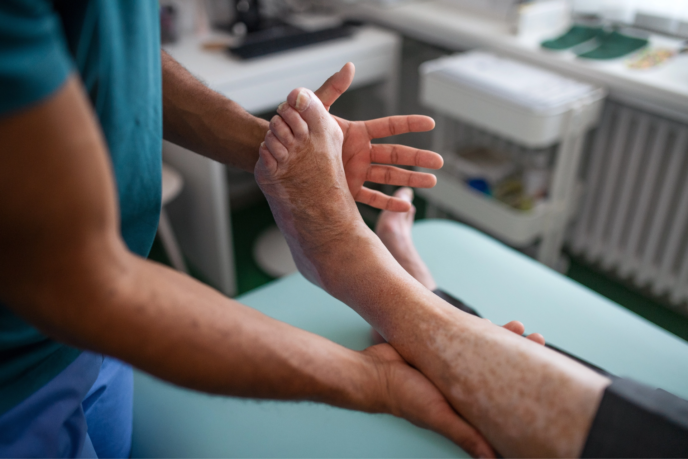
What is Peripheral Artery Disease?
Peripheral Artery Disease (PAD) is a circulatory system condition caused by the gradual buildup of cholesterol plaque in the arteries. Though PAD can occur anywhere in the endovascular system, it frequently occurs in the legs. Over time, the accumulation of plaque—a combination of cholesterol, fat, calcium, and other substances coursing through the bloodstream—on the walls of the arteries can cause them to narrow.
As a result, it becomes more difficult for blood to freely flow to the legs and feet. Often patients with peripheral artery disease have a much higher risk of developing serious health problems, including heart attack, stroke, or even amputation. Peripheral Artery Disease is common and treatable. The key is recognizing the warning signs so PAD can be treated early before it progresses.

In the early stages, 66% of all PAD patients have NO Symptoms. Typically, symptoms won’t appear until your arteries narrow by 70%, or until you experience claudication. It’s important to know the signs and symptoms of peripheral artery disease so you can catch it early and prevent it from becoming worse later on.
PAD Symptoms
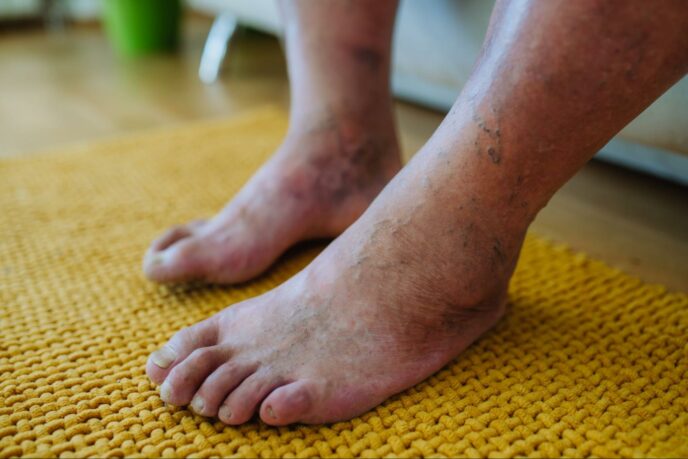
- Leg Pain
- Leg Discoloration
- Leg Numbness
- Leg Weakness
- Non-Healing Foot Wounds
- Poor Circulation
Risk Factors of Peripheral Artery Disease
An estimated 8.5 million people have peripheral artery disease in the United States. Women and men are both affected by PAD, but African Americans have approximately twice the risk of PAD as Caucasians or Asian Americans. A better understanding of peripheral artery disease risk factors can help you make lifestyle changes to reduce your chances of developing the disease.
PAD Risk Factors
- Age Above 50 years
- Diabetes
- High Blood Pressure/Cholesterol
- History of Vascular Disease
- Kidney Disease
- Obesity
- Race
- Smoking
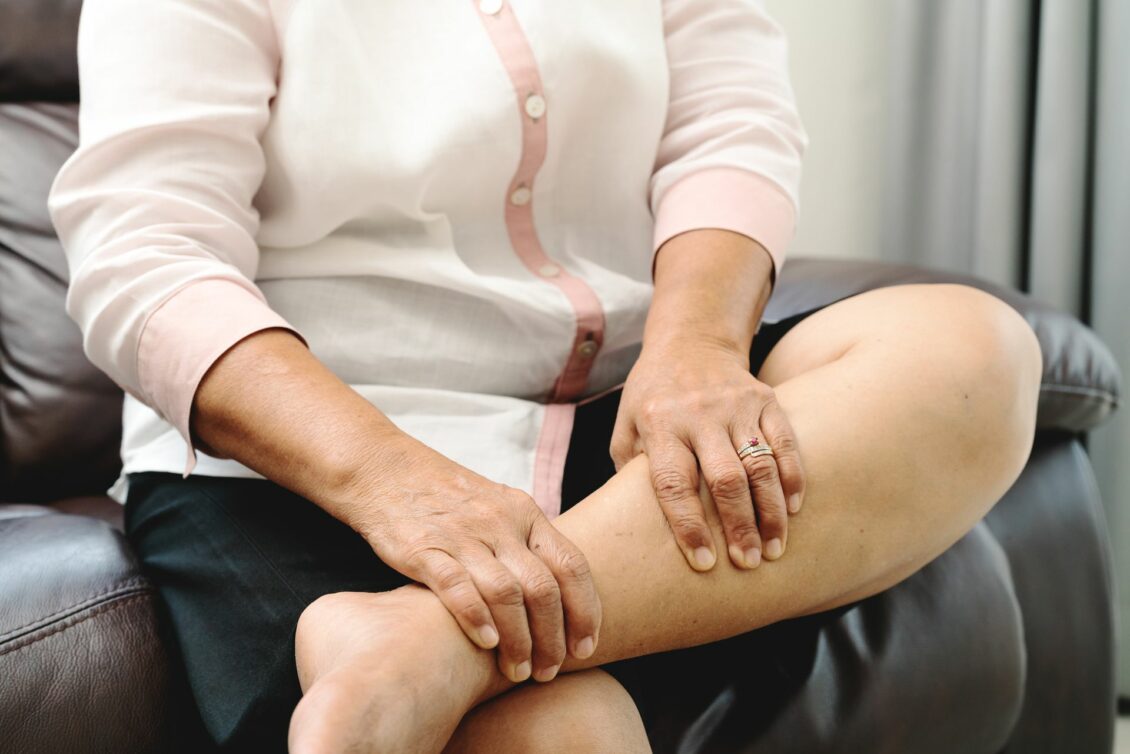
The main cause of peripheral artery disease is atherosclerosis, which is a health condition that causes the narrowing of arteries due to a plaque buildup. Atherosclerosis can also cause the arteries to become blocked, resulting in not enough blood, oxygen, or nutrients to travel to the legs or feet. There are also less common causes of PAD that may lead to the disease, involving injury, inflammation, or exposure to radiation.
Causes of PAD
- Atherosclerosis
- Blood Vessel Inflammation
- Injury to the Legs
- Leg Weakness
- Muscles or Ligament Changes
- Radiation Exposure
Stages of Peripheral Artery Disease
There are four different stages of PAD. Your vascular specialist will determine if you have any of the following stages at the time of your screening.
Asymptomatic
Not everyone experiences symptoms of PAD in the early stages. Patients during the first stage do not have symptoms even though the disease may keep progressing unnoticed until symptoms occur.
Claudication
Stage two of PAD is claudication. Patients during this stage begin to feel discomfort and pain in their lower extremities, which can occur during any type of exercise and go away after the patient rests.
Critical Limb Ischemia
The third stage of PAD is known as Critical limb ischemia (CLI), which severely reduces the blood flow to the extremities. During this stage, patients feel intense pain in the legs and feet even while resting (without any activity such as sitting in a chair, laying down or when sleeping).
Acute Limb Ischemia
Acute Limb Ischemia (ALI) is the final stage of PAD, involving the sudden loss of blood to the lower extremities. At this stage, patients can experience significant pain and their limbs can rapidly deteriorate and turn cold and pale -(which can lead to) leading to paralysis, amputation, or sometimes death.

Peripheral Artery Disease Diagnosis
There are multiple ways to diagnose PAD. One of our affiliated specialists will perform a physical examination, review your medical history, and assess your risk factors. They may order different noninvasive tests to help diagnose the disease and determine its severity.
PAD Diagnostic Tests
- Ankle-Brachial Index (ABI)
- Angiography
- CT Angiography
- Blood Tests
- Duplex Ultrasonography
- Magnetic Resonance Angiography (MRA)
Peripheral Artery Disease Treatment
The American Endovascular affiliated team of vascular specialists is at the forefront of the detection and treatment of PAD. They have a proven track record of success at preventing the progression of PAD, saving the limbs that others can’t. Their array of minimally invasive-image guided treatment options can restore blood flow and get you on the road to a healthier life.
Amputation Prevention
Using advanced techniques and technologies, such as pedal loop interventions, our affiliated physicians help with limb salvage and preservation in patients with non-healing wounds due to peripheral artery disease.
Angioplasty
Angioplasty uses a low-profile catheter with an inflatable balloon to stretch the affected artery open. The primary goal of the procedure is to restore blood flow to the clogged artery and increase oxygen-rich blood to the body’s muscles and tissues.
Atherectomy
An atherectomy involves removing plaque from arteries with a catheter via a minimally invasive incision. This procedure has evolved with cutting-edge advances, including orbital, rotational, and diamond-coated surface technology, as well as a laser to remove or modify plaque from a clogged blood vessel.
Stent Placement
Stents are a host of different metallic-based implantable devices inserted into the artery to provide a new skeletal framework to strengthen the walls and help it remain open. Some stents may have drug-eluting properties to prevent blood clotting and increase longevity.

What to Expect from
Your PAD Treatment
Peripheral Artery Disease FAQ
The first symptom of PAD is generally leg, calf or foot pain during physical activity, such as walking, that gets better after you rest. You may experience pain, aches, or cramping in your thighs or calves or feet during your walk, which may be a sign of PAD.
Smoking is the most common risk factor for PAD. 80% of people who smoke tobacco or used to smoke have PAD. Smoking can bring on PAD symptoms almost 10 years earlier and significantly increase the risk of the disease due to causing impaired blood flow in the body.
Peripheral arterial disease is reversible in the earlier stages. You can reverse PAD symptoms by controlling your cholesterol and blood pressure levels with medication and through lifestyle changes such as diet, exercise, or quitting smoking.
Our Vascular Specialists
American Endovascular is proud to be affiliated with vascular specialists in NY and NJ that represent the “best of the best.” Our affiliated physicians at our vascular centers are nationally recognized as innovators and leaders in vascular and interventional radiology, providing high-quality and compassionate care for our patients living with PAD.
Recent Blogs & Videos
Learn more about vascular health, prevention, and care for Peripheral Artery Disease.