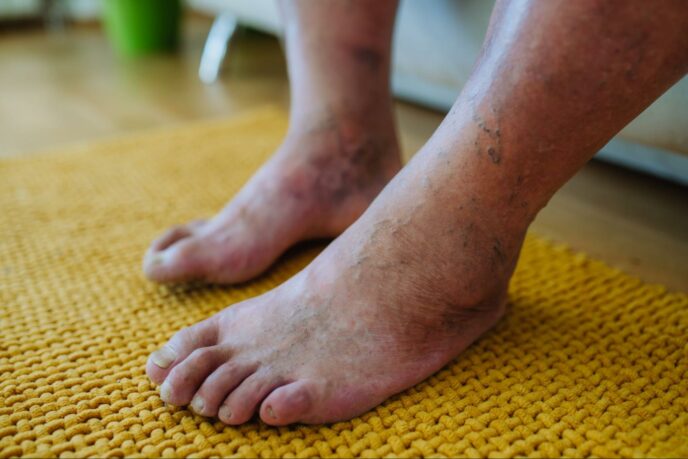
Arterial Ulcers vs Venous Ulcers
Diabetic foot ulcers and leg ulcers can sometimes be asymptomatic. So how will you know when you are in need of medical advice? It is important to know what the symptoms of a diabetic foot ulcer are, the difference between arterial and venous ulcers, and what causes them.
What are the symptoms of a diabetic foot ulcer?
Not all diabetic foot ulcers are symptomatic. Patients that suffer from severe diabetes may not even know that they have a foot ulcer because of various problems with sensation and paresthesias and neuropathy, until it is identified at a follow-up visit or is noticed later on. Presenting symptoms may include pain, a malodour, discoloration, or gangrene, which are usually clear signs of a diabetic foot ulcer.
What is the difference between arterial and venous ulcers?
Arterial and venous ulcers can occur separately or simultaneously. In patients who have arterial disease and arterial ulceration, there’s often also a venous component and vice versa. We call that combined arterial and venous insufficiency. Specifically, there is a typical location and a typical look for venous ulcerations, this is usually above the ankle bone on the inside of your leg. That’s usually a result of several problems, one of them being venous insufficiency. Arterial ulcerations are related to poor blood flow, presenting in patients with diabetes and patients who smoke regularly. Those are usually seen on the toes or on the feet. Both venous and arterial ulcers can be painful. Venous wounds can be more painful than arterial wounds, but both have the ability to cause pain, and it can be very difficult to tell the difference. A podiatrist and vascular specialist are really key in the diagnosis and establishing further treatment options and diagnostic imaging type testing.
What is the main cause of arterial ulcers?
One of the main causes of arterial ulceration is the lack of blood flow, but this may not have caused the ulcer initially. The lack of blood flow is the reason the ulcer does not heal. Often, the cause of ulceration is simply bumping one’s foot causing a small cut, cutting the toenail bed a little bit too close, stepping on a piece of glass, or a sharp object breaking the skin of the feet. The poor blood circulation and lack of good blood supply to that wound area is what allows the wound to progress and to become a non-healing diabetic-type ulcer. Other factors including the amount of sugar that’s in the body and continuing to smoke will delay or almost negate any significant wound healing. That is why it is very important to try to resolve all of these issues with a multifaceted approach.
What are the treatment options for arterial ulcers and venous ulcers?
There are multiple treatment options available for both arterial and venous ulcers. Starting with identifying the cause, treatment options include trying to maintain a healthy diet, decreasing Hemoglobin A1c in patients with diabetes, and ceasing smoking in patients who continue to smoke. Open wound care is crucial, especially debridement and removal of any type of infection that may be present. When it comes to other procedural treatments for either arterial or venous ulcers, or combined arterial and venous ulcers, you have to identify the problem. If there is an arterial flow problem, meaning not enough arterial blood circulation coming down towards that wound base, there are several treatment options to try to open up those blood vessels, including an endovascular approach. This approach usually requires an angiogram and some sort of re-vascularization, either using a balloon, an atherectomy type of device to clear the plaque, or a stent to prop open that blood vessel.
Additionally, venous stasis ulcers usually need some sort of compression therapy, whether it be mechanical compression, an Unna boot type wrap, or similar, which is typically applied cool or cold by the wound care center or at the podiatry clinic. Additionally, if identified for venous insufficiency, either in the greater saphenous vein, which is the area where people tend to see those bulging varicose veins, or in the lesser saphenous vein, there are ways to close that vein down, with certain types of medication, laser, or other treatment options.
Other aspects of the venous ulcer can be seen in patients suffering from edema or fluid in the soft tissues. The main treatment option there is to treat those superficial veins. We tend to also look at the deep veins, to see if there are any blood clots, or if the blood flow returning towards the heart is abnormal. There are options to propagate that blood flow to go back toward the heart and decrease the edema and swelling in that area.
Related Blogs & Videos
Learn more about vascular health, prevention, and care for Peripheral Artery Disease.