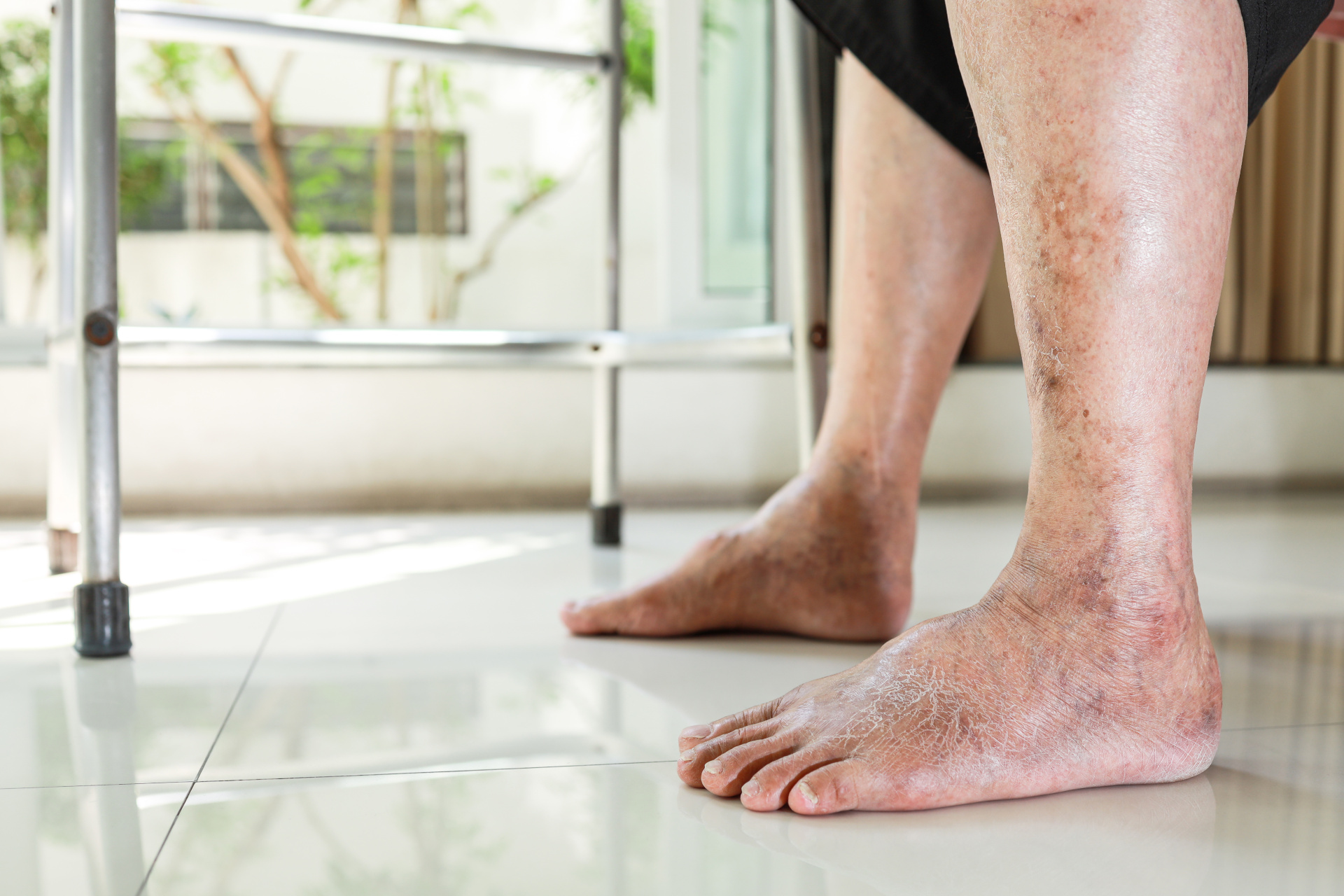
What is Peripheral Artery Disease
Peripheral Artery Disease (PAD) is a condition caused by a plaque buildup in the arteries of the legs, restricting blood flow to the lower extremities. Elderly patients and cigarette smokers are particularly at risk. But perhaps the most at-risk population for PAD are patients with diabetes mellitus. It is important that patients with diabetes be aware of the warning signs and symptoms of PAD so it can be treated early before foot ulcers or other serious conditions develop.
What is the Correlation Between Diabetes and Peripheral Artery Disease?
Diabetes is known to significantly increase the risk of developing Peripheral Artery Disease. In fact, studies show that one out of every three adults over 50 with diabetes is likely to have Peripheral Artery Disease. One of the most common manifestations of PAD in diabetics is the development of a foot or toe ulceration. Ulceration—a slowly-healing open sore on the foot or toe which may be superficial or may extend into the tendons and bones—is a serious condition and requires prompt medical attention. In 2019, between 1 to 3.5 million Americans have had a history of foot ulceration.
According to the American Diabetes Association, the risk of diabetic patients developing a foot ulcer in their lifetime is as high as 25%. Unfortunately, since the number of patients with diabetes is increasing every year, the occurrence of diabetic foot ulcers is expected to increase.
What PAD Symptoms Do Patients with Diabetes Need to Watch for?
American Endovascular’s Dr. Joseph Shams is one of the nation’s most experienced and respected Endovascular Surgeons. He has treated countless patients with Peripheral Artery Disease, many of whom are long-term diabetics.
Dr. Shams says one of the most common manifestations of diabetes is peripheral neuropathy—a feeling of numbness/weakness—usually manifesting in the feet or toes. For patients with Peripheral Artery Disease, this condition can be extremely dangerous as it may mask the early signs of PAD, such as pain in the calf when walking or rest pain within the toes. As Dr. Shams said, “Diabetic patients are at significant risk since even benign skin infections or sores may progress very quickly to full-blown soft tissue or bone infections.”
Dr. Shams went on to say, “For some diabetics, peripheral neuropathy can mask all the usual warning signs that accompany Peripheral Artery Disease. The most extreme example I recall is when a diabetic patient stepped on a nail and wasn’t aware. The nail was actually deeply embedded in his foot. But due to advanced neuropathy, he couldn’t feel a thing. He developed a severe infection at the site of the wound but had no symptoms.”
Why Does Diabetes Cause So Many Foot Problems?
Diabetics have high blood sugar levels. Over an extended period of time, this can cause damage to nerves or blood vessels. Nerve damage from diabetes may lead to numbness or loss of feeling within the feet or toes. Because the legs and feet have smaller blood vessels, they are more susceptible to blockage. In terms of circulation, the feet get the least amount of blood flow—they are literally the “end of the road.” And because neuropathy can often numb the feet of diabetics, they may not be aware that anything is even wrong until it’s too late.
This is why it’s of the utmost importance for patients with diabetes to schedule an endovascular screening.
I Don’t Have Diabetes. How Can I Tell If I Have Peripheral Artery Disease?
The most common symptom of Peripheral Artery Disease (PAD) is a pain in the back of the legs that occurs while walking. This pain is known as claudication, and it is caused by a lack of blood flow to the legs due to arteries blocked by plaque. What is plaque? It’s a deposit in the wall of the blood vessel composed of fat, cholesterol, calcium, and other substances. It may develop slowly over a person’s lifetime but when it reaches a critical point it can block off the blood vessels and cause claudication symptoms.
In milder PAD cases, the claudication subsides when resting. In more advanced cases, the pain moves to the toes and is present even at rest, particularly at night. It’s not uncommon for PAD sufferers to drape their legs down the side of the bed in order to relieve pain and increase blood flow to the feet.
Other common PAD symptoms include:
- Coldness/numbness within the toes
- Discoloration of the feet or toes
- Severe pain
- Slowly-healing wounds
What are the Warning Signs for Peripheral Artery Disease?
Over the course of his distinguished career, Dr. Shams has treated countless patients suffering from Peripheral Artery Disease. Based on what he sees, one situation is the most dangerous of all.
“The biggest red flag for Peripheral Artery Disease is rapid progression. If someone was walking around normally a week ago, and now can barely get around, that is a dangerous warning sign. Acute onset discoloration, along with severe pain in the toes, also indicates an advanced case of Peripheral Artery Disease.”
-Dr. Joseph Shams, MD
What are the Most Common Misconceptions About Peripheral Artery Disease?
Because Peripheral Artery Disease is very common with patients in their 70s and 80s, many danger signs can be overlooked. As Dr. Joseph Shams says, “Quite often, patients don’t think they have a problem. They may only experience symptoms when they’re walking up the stairs, so they think they’re just out of shape, or consider it to be just a natural part of the aging process.”
The truth is, pain in the legs is not a natural part of the aging process. It’s a warning sign—your body telling you that something’s wrong. Without sufficient blood flow to the legs, Peripheral Artery Disease will only get worse.
What’s the Difference Between Arteries and Veins?
Another common misconception of Peripheral Artery Disease stems from a common confusion between arteries and veins.
- Arteries carry blood from the heart to the rest of the body.
- Veins return the blood back to the heart.
As its name suggests, Peripheral Artery Disease is a condition caused by a plaque buildup in the arteries. Conditions of the veins, such as bulging, varicose veins, or swollen legs—while concerning—are usually not indicators of Peripheral Artery Disease.
If you or someone you know is experiencing pain in the legs, slowly-healing leg wounds, or coldness/numbness in the legs or feet, you may be suffering from the early stages of PAD.
What Steps can People Take to Help Avoid Peripheral Artery Disease?
In some cases—particularly for elderly patients—the onset of Peripheral Artery Disease may not be preventable. But for the rest of the population, particularly those with diabetes, it’s critical to be proactive. Here are 5 easy things anyone can do to help prevent the spread of Peripheral Artery Disease.
- Stop Smoking
Smokers are 2-3X more likely to develop Peripheral Artery Disease than non-smokers. In general, they develop symptoms at an earlier age than non-smokers. Typical symptoms include claudication in the thigh or buttocks. Male smokers can also develop sexual side effects such as impotence. If you currently smoke, quitting is the best thing you can do to prevent the onset of PAD.
- Get Exercise
The best exercise for combating PAD is also the simplest: walking. Swimming is also very effective.
- Weight Loss
The overweight population is more at risk of developing PAD. Besides the other health benefits, weight loss can promote better circulation in the legs and feet.
- Take Care of Your Feet
Do your best to avoid any injuries to your feet or toes. Ingrown toenails in particular can be dangerous as they are prone to infection. It’s important to see your podiatrist regularly, particularly for elderly patients.
- Schedule an Endovascular Screening
If you or someone you know has symptoms of PAD—particularly if you have diabetes—it’s important to schedule an arterial ultrasound study. That’s the most reliable way to detect any plaque buildup in the feet or legs.
How Can American Endovascular Treat Peripheral Artery Disease?
Thanks to recently-developed, non-surgical, minimally invasive procedures, PAD patients are living longer and healthier lives. According to Dr. Shams, in just the last decade, significant technological and medical innovations have made Peripheral Artery Disease easier to detect and treat.
“In the past, the only way to treat PAD was via surgical bypass. A synthetic graft would be inserted above the blockage and connected to an open blood vessel further down the leg, bypassing the blockage. This was frequently a complicated procedure with a prolonged recovery time. In addition, success rates weren’t great. But with the newer endovascular techniques like Atherectomy, there’s no incision, or hospital stay. Most procedures take about an hour, and the success rate is higher as compared to bypass operations.”
-Dr. Joseph Shams, MD
The team of vascular specialists at American Endovascular are at the cutting edge of endovascular treatment. Our doctors have pioneered the use of new techniques and technologies that can help PAD sufferers lead more normal lives without the need for open surgery.
What is an Atherectomy and How Can It Help with Peripheral Artery Disease?
At the forefront of this revolution in PAD care is Atherectomy. Here’s how it works:
- A small incision is made in the patient’s artery, usually at the groin
- A catheter fitted with a tiny rotating burr is threaded down to the blocked vessel
- The burr spins incredibly rapidly, at approximately 80,000 RPM in order to shave the plaque into microscopic bits
- Because the burr spins at such high speeds, it obliterates the plaque instead of simply pushing it further down the leg
Atherectomy is a non-surgical, minimally invasive endovascular procedure that lasts about an hour. Patients are asleep during the procedure, and recovery times are short.
Why is American Endovascular’s Success Rate so Much Higher than Everyone Else?
Simply put, American Endovascular saves the limbs that others can’t. We have been able to save more than 80% of patients’ limbs after being told they needed an amputation. What’s behind our astounding success? Our world-class team of doctors. They handle the most complex, most difficult cases—the ones others are afraid to treat.
Dr. Joseph Shams is a pioneer in one of the most complex procedures for advanced PAD. Instead of threading the catheter from the groin down, he and the rest of his American Endovascular team can treat blockages from below! This is particularly helpful for diabetics. As he explains,
“Diabetics often get PAD in the upper calf, affecting all 3 major arteries in that region. If you attack the blockage from below, entering from the top of the foot or the ankle, you can reach the blocked blood vessels more easily.”
-Dr. Joseph Shams, MD
Don’t let Peripheral Artery Disease Ruin Your Quality of Life
As you’ve seen, there are many simple things you can do to help control PAD. Smoking cessation, weight loss, exercise, and proper foot care are critical to your vascular health. But sometimes, the only solution is medical. That’s where American Endovascular is uniquely qualified to help.
If you, or someone you know, is experiencing debilitating symptoms of PAD, request an appointment with American Endovascular today. We have the experience, team, and technology needed to fix clogged arteries and treat peripheral artery disease.
Related Blogs & Videos
Learn more about vascular health, prevention, and care for Peripheral Artery Disease.




