What is Dialysis Access Management?
For the more than 475,000 patients requiring life-saving dialysis treatment, access is everything. If a graft or fistula is blocked or even somewhat obstructed, it could lessen the amount of dialysis received. That could seriously jeopardize a patient’s health, and even shorten their life span.
American Endovascular affiliated centers enable qualified medical professionals to provide a range of minimally invasive-image guided dialysis access management procedures. These procedures are to manage and prolong the life of dialysis access grafts and fistulas, so patients can get the dialysis treatment they need without anything getting in the way.
How Does Dialysis Work?
End-Stage Renal Disease (ESRD) occurs when the kidneys no longer function as they’re supposed to. The job of the kidneys is to remove excess waste products and fluids from the body, as urine. When kidney failure occurs, these substances have nowhere to go. They build up in the bloodstream which can cause a range of life-threatening conditions, to nearly every part of the body.
Dialysis treatment is designed to replicate the function of the kidneys, cleaning impurities, and excess fluid from the blood. Dialysis begins with the creation of an access—a point where the dialysis system can connect to the patient’s bloodstream. The following are three common methods of dialysis treatment.
AV Fistula
An AV fistula is a surgically created connection between the artery and the vein. This is the preferred method, as it is 100% original tissue, which means a fistula can resist clotting and infection.
AV Graft
An AV graft is a small tube—an indirect connection between an artery and a vein via a plastic tube or possibly a donated cadaver artery.
Hemodialysis Catheter Placement
A vascular specialist utilizes ultrasound fluoroscopic images to precisely place a catheter through the major vein (preferably jugular) to allow removal of blood to be cleared with the hemodialysis machine then replaced back into the venous system with the blood that has been cleansed. This catheter should be considered as a temporary catheter to final access creation or renal transplant.

How Does Dialysis Access Management Work?
When AV fistulas or grafts malfunction—usually as a result of narrowing or blockage due to frequent use—American Endovascular affiliated physicians can help remedy the problems using an array of minimally invasive procedures designed to restoring blood flow and prolong the longevity of the access so dialysis can continue.
Dialysis Access Procedures Performed by American Endovascular Affiliated Physicians
American Endovascular’s affiliated vascular centers offer multiple treatment options to prolong the life of fistulas and grafts, diminishing the need to put patients through multiple access surgeries. Our affiliated physicians specialize in complex endovascular care and are leading experts in dialysis access management. They know what it takes to help medical professionals treat dialysis patients and lead longer, more comfortable lives. Procedures include:
Fistula Maturation
After a fistula is surgically created, the artery and veins experience new hemodynamic forces that cause a change in blood flow. As a result, the blood vessels change in diameter and arterial walls become thickened to accommodate the new blood flow. This remodel is known as fistula maturation. However, there are times when the newly created fistula does not remodel as it should. When that happens, physicians can employ a range of endovascular techniques such as angioplasty to help the fistula get to the place it needs to be in order to handle the endovascular demands of dialysis.
Dialysis Catheter Placement
Certain times, due to age, health, or other factors, a patient is unable to receive a fistula or graft. When that occurs, physicians can insert a permanent or temporary catheter— providing direct access for dialysis—in either the chest or top of the thigh.
Thrombolysis & Thrombectomy
There are times when fistulas and grafts can narrow and become thrombosed due to a buildup of blood clots from routine use. Physicians can work to clear the blocked access using thrombolysis and thrombectomy. Thrombolysis involves injecting a medicine into the clogged access, breaking down and dissolving the clots. Thrombectomy is a minimally invasive endovascular procedure where the blood clot is physically removed, or macerated, clearing the access for dialysis treatment.
Angioplasty & Stenting
One of the most common treatments for fistulas and grafts is angioplasty. An area of narrowing can occur in the fistula or graft due to regular use. Angioplasty works to stretch the narrow portion of the access by inserting a catheter with a small balloon and inflating it to reopen the vessel. This treatment restores optimal flow so the patient can receive dialysis treatments. In situations where angioplasty is not effective, a stent—a small wire mesh tube—is inserted to keep the vein or artery open, optimizing flow in the access.
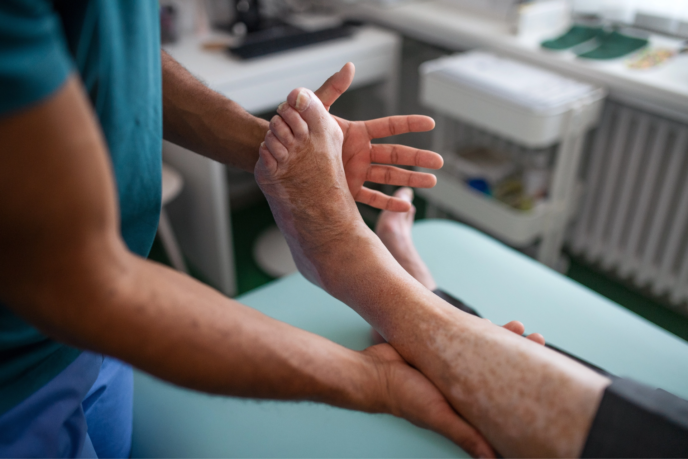
AV Fistula Banding
AV Fistula Banding is a technique performed by licensed physicians on patients with Steal Syndrome. This syndrome, occurring in roughly 1% of fistulas and 5% of grafts, occurs when a fistula or graft has such high blood flow that it can actually “steal” blood from the hand, causing numbness and pain. Banding lowers the blood flow in the fistula, delivering more blood to the hand.

What to Expect from
Dialysis Access Management
Dialysis Access Management FAQ
There are three different types of vascular access that can be placed for hemodialysis. They are called a fistula, a graft, and a catheter.
Whether your vascular access is a fistula, graft or catheter, you need to make sure you take care of it. With a fistula or graft, you want to make sure that you wash them with antibacterial soap before dialysis. You also want to check for redness on any area of your access and report it to your care team. With a catheter, you want to ensure that the catheter dressing is kept clean and dry. Also, you want to make sure that the access is cleaned and the dressing is changed by your team at each dialysis visit.
In terms of overall performance, an AV fistula is often considered the “gold standard” for vascular (hemodialysis) access. It is associated with fewer infections and fewer hospitalizations since it tends to last longer than other access types.
Our Vascular Specialists
Our affiliated vascular specialists perform dialysis access management for patients in New York and New Jersey.
Recent Blogs & Videos
Learn more about vascular health, prevention, and care for Peripheral Artery Disease.