Why Are My Feet Purple?
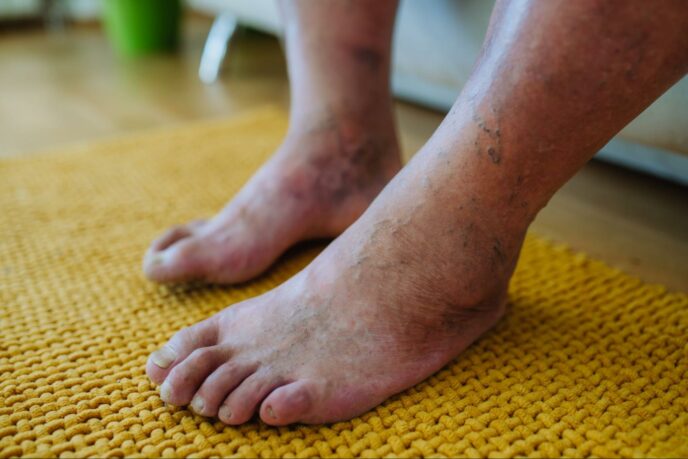
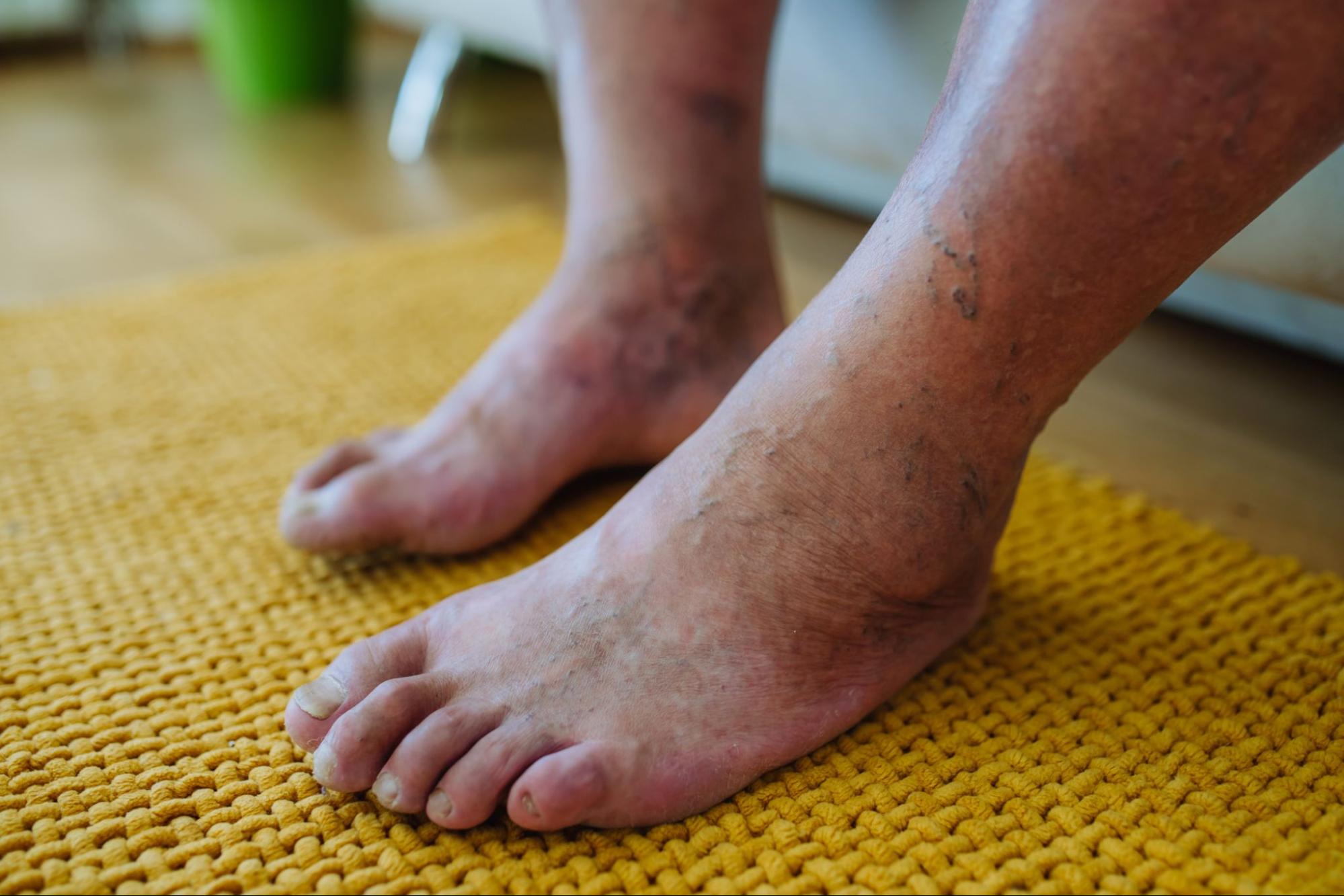
Have you ever looked down at your feet and noticed a strange discoloration, perhaps a purple hue that seems out of place? While it might be alarming at first glance, there’s often an underlying condition causing your purple feet, which could be Peripheral Artery Disease (PAD). In this article, we’ll dive into some of the potential causes of purple feet, why PAD may cause purple feet, and explore possible treatment options.
Purple Feet Causes
Diabetes
Diabetes is a common cause of purple feet, particularly in individuals with poorly controlled blood sugar levels. Over time, high blood sugar can damage the nerves and blood vessels in the feet, leading to a condition known as diabetic neuropathy. Diabetic neuropathy can cause numbness, tingling, burning pain, and changes in skin color, including a purple discoloration due to poor circulation.
Foot Injuries
Injuries to the feet are common and can lead to discoloration known as bruising. Bruises can appear blue, yellow, green, or purple, depending on the severity of the injury, such as a sprain or a broken bone in the foot or ankle.
Raynaud’s Disease
Raynaud’s disease is a condition that causes reduced blood flow to the extremities, typically triggered by cold temperatures or stress. The feet may turn white, then blue or purple, before returning to their normal color as blood flow improves. People with Raynaud’s disease may also experience a change in sensation, such as a numbing or tingling feeling, associated pain, or struggles with coordination and movement in their toes.
Venous Insufficiency
Venous insufficiency occurs when the veins in the legs have difficulty returning blood to the heart. This can lead to blood pooling in the feet and ankles, causing them to appear purple or blue. Factors such as obesity, pregnancy, and prolonged sitting or standing can make venous insufficiency symptoms worse.
Peripheral Artery Disease (PAD)
Peripheral artery disease is a condition that narrows or blocks the arteries that supply blood to the extremities, most commonly the legs and feet. When blood flow to the feet is compromised due to PAD, it can result in various symptoms, including pain, numbness, tingling, and changes in skin color. The reduced blood flow may lead to a bluish or purplish discoloration of the feet, especially during periods of rest or activity.
Does PAD Cause Purple Feet?
Yes, skin discoloration is one of the most common symptoms of PAD. Reduced blood flow caused by PAD can lead to changes in the color of your skin on the legs and feet, which can make the skin appear purple or blue. If you’re experiencing purple feet due to PAD, here are some possible explanations:
Poor Circulation
PAD causes poor circulation, which restricts blood flow to the legs and feet. As the arteries in your lower extremities become narrowed or blocked by a buildup of plaque (atherosclerosis), the flow of oxygen-rich blood to the feet is restricted, causing the skin to appear purple or blue.
Peripheral Cyanosis
The discoloration of the feet, often turning purple or bluish, is a result of insufficient oxygen supply to the tissues, a condition known as cyanosis. Cyanosis occurs when the blood lacks oxygen, causing the skin to appear bluish or purple. In the case of PAD, restricted blood flow to the legs means that oxygen-rich blood struggles to reach the feet adequately. As a result, the tissues become starved of oxygen, leading to cyanosis and the characteristic purple hue.
Blood Pooling
Another reason for purple feet in PAD is blood pooling. When there is a restriction in arterial blood flow, the return of blood to the heart becomes more difficult, which can result in blood accumulating or pooling in the feet and ankles. Due to the blood being deprived of oxygen, the skin turns even more purple.
Delayed Healing
Poor blood flow also slows down your body’s ability to heal wounds or injuries. If you have PAD, even minor cuts or sores on your feet may take longer to heal and can become infected easily. As a result, this can make the discoloration worse on your feet and lead to a purple appearance.
What are the other Symptoms of Peripheral Artery Disease in the Feet?
Purple feet can be a sign of PAD, along with other symptoms in the legs or feet, such as:
- Numbness or Weakness: Reduced sensation or weakness in the legs or feet, often felt during movement or while at rest.
- Coolness or Cold Sensation: The feet may feel cooler to the touch than other parts of the body due to decreased blood flow.
- Skin Changes: Besides purple discoloration, PAD can lead to other skin changes such as dryness, thinning, shiny appearance, or a lack of hair growth on the feet and legs.
- Slow Wound Healing: Wounds, cuts, or sores on the feet may take longer to heal than usual or may not heal properly due to reduced blood flow.
- Decreased Pulse: The pulse in the feet or legs may be weak or absent, particularly in advanced cases of PAD.
- Foot Ulcers: Non-healing wounds or ulcers, especially on the toes, feet, or heels, which can become infected and may lead to tissue damage or gangrene if left untreated.
- Foot Pain at Rest: In severe cases, individuals may experience pain or discomfort in the feet or toes even while resting, which is known as ischemic rest pain.
- Changes in Nail Growth: Slower nail growth or changes in the appearance of toenails, such as thickening or discoloration, may occur.
Preventing and Treating Peripheral Artery Disease
Fortunately, there are various treatment options for PAD, including lifestyle changes and minimally invasive procedures to treat and prevent it from getting worse.
Lifestyle Changes
- Quit Smoking: Smoking is a major risk factor for PAD as it damages blood vessels and accelerates the progression of the disease. Quitting smoking is essential to slow down the condition and reduce the risk of complications.
- Healthy Diet: Adopting a balanced diet low in saturated fats, cholesterol, and sodium can help manage PAD by controlling blood pressure and cholesterol levels. We recommend Incorporating plenty of fruits, vegetables, whole grains, and lean proteins into your diet.
- Regular Exercise: Exercise, such as walking or cycling, can improve circulation, alleviate claudication symptoms (leg cramping), and enhance overall cardiovascular health.
- Weight Management: Maintaining a healthy weight reduces the strain on the cardiovascular system and lowers the risk of complications associated with PAD.
Medications
Your doctor may prescribe medications to manage symptoms and reduce the risk of complications associated with PAD. These medications may include cholesterol-lowering drugs, blood pressure medications, and medications to improve circulation.
Foot and Wound Care
If you have PAD, maintaining proper foot hygiene and care is essential to avoid complications such as ulcers and infections. This involves inspecting the feet regularly for signs of injury, keeping the skin moisturized, wearing comfortable shoes, and avoiding activities that could harm the feet. If you have PAD-related ulcers or wounds, specialized wound care may be necessary to promote healing and avoid infections.
Minimally Invasive Treatments
If the combination of lifestyle changes and medications is still not improving your PAD symptoms and foot discoloration, there are minimally invasive treatment options that can help. At American Endovascular, we offer angioplasties and stent placements to widen narrowed arteries and improve blood flow and an atherectomy procedure to remove plaque from the arteries. These image-guided treatments are same-day procedures that do not require a hospital stay and offer a quicker recovery time with high success rates.
Prevent PAD and Purple Feet with American Endovascular
If you are experiencing purple feet along with other uncomfortable PAD symptoms, American Endovascular can help. Our affiliated vascular surgeons take the time to understand your specific case by carefully reviewing your medical history, conducting a detailed assessment, and creating an appropriate treatment plan. Contact us today to schedule an appointment so that we can help you get back on track.
Related Blogs & Videos
Learn more about vascular health, prevention, and care for Peripheral Artery Disease.