Our physicians are some of the world’s most respected vascular experts.
Tackling the Most Complicated PAD Cases
American Endovascular has brought together some of the industry’s top vascular specialists for one reason: to help them save lives. Our affiliated team of physicians use the latest and most advanced minimally invasive-image guided endovascular techniques and technologies currently available anywhere to bring life and hope to their patients with peripheral artery disease (PAD).
PAD is a circulatory system condition caused by the gradual buildup of plaque in the extremity arteries. Though PAD can occur in the arms, it is most often found in the arteries of the legs. You can rest assured that the American Endovascular team of affiliated physicians is unsurpassed in its knowledge and technical expertise in PAD and amputation prevention.
Trust American Endovascular to:
Provide world-class amputation prevention care for patients with PAD.
Serve as the primary go-to limb salvage resource for doctors before scheduling amputations.
Undertake highly complex procedures for peripheral artery disease and critical limb ischemia that others cannot do.
Offer the most innovative endovascular procedures including the treatment of peripheral artery disease, critical limb ischemia, and amputation prevention.

Are You Experiencing PAD Symptoms?
In the early stages, PAD can present no symptoms at all. However, when symptoms do occur, they can be disruptive to everyday life and lead to complications. The key is to recognize the warning signs of PAD, so it can be detected and treated early before it progresses. Symptoms of PAD can be caused by various conditions, which is why it’s important to work with a vascular specialist if you suspect you may have these common symptoms.
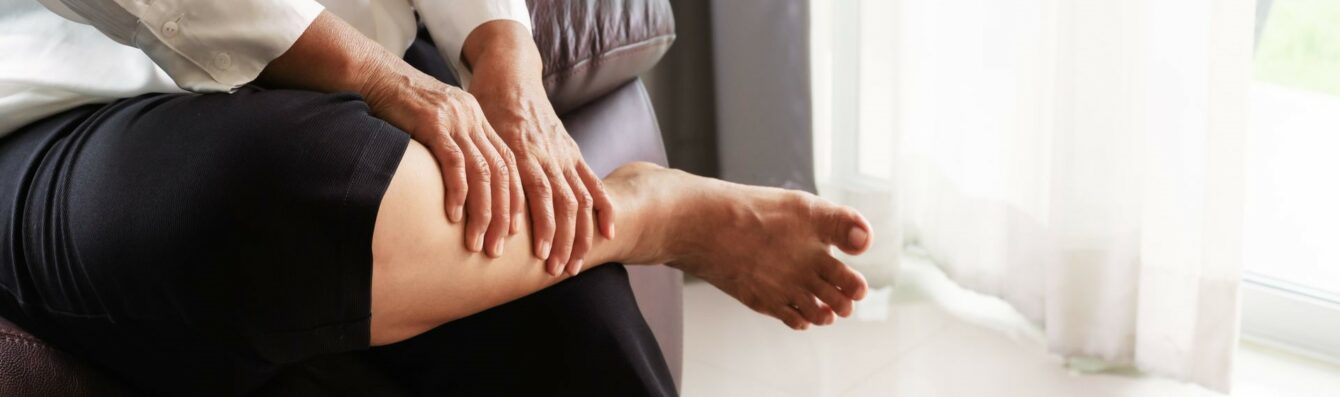
Leg Pain
A classic symptom of PAD is feeling pain in your legs during physical activity that gets better after rest.
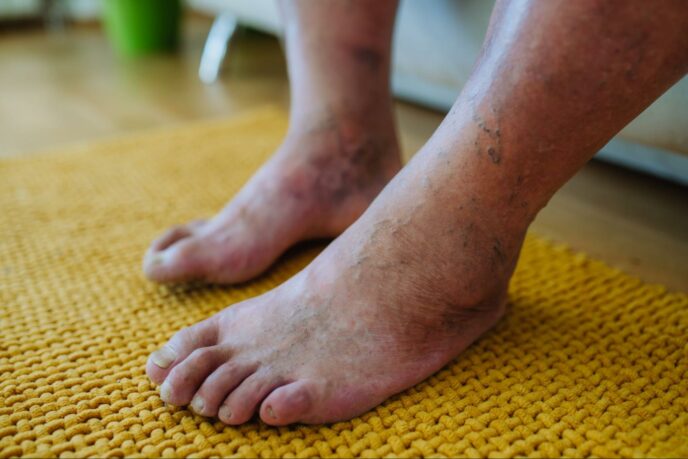
Leg Discoloration
PAD may cause the color of your feet and legs to change to a purple or blue color due to poor circulation.
Leg Numbness
You may feel a numbness or tingling sensation in your legs or feet as a sign of PAD.
Leg Weakness
Feeling a weakness in one or both of your legs that impacts standing may be a sign of a more advanced case of PAD.
Non-Healing Wounds
Non-healing wounds on your feet or legs is a serious and more advanced sign of PAD.
Poor Circulation
PAD restricts the blood flow in the arteries of legs, leading to poor circulation.
We Offer Minimally Invasive Treatments for PAD
PAD treatment has taken a great leap forward over the past years. New endovascular technologies and procedures available can significantly improve the lives of those living with PAD. American Endovascular’s affiliated team of physicians has successfully prevented the progression of PAD with minimally invasive-image guided treatment options. Our affiliated physicians have a proven and extraordinary track record of saving their patients’ limbs after they were told they needed an amputation. If you are dealing with debilitating and uncomfortable symptoms, our treatments for PAD are the best way to get relief without the risks of invasive surgery or amputation.
Atherectomy
An atherectomy removes plaque buildup in the arteries using a catheter.
Angioplasty
An angioplasty uses a balloon to stretch open a narrowed or blocked artery.
Amputation Prevention
Our vascular centers use advanced techniques and technologies, such as pedal loop intervention, to help patients with more severe PAD cases avoid amputation.
Stent Placement
A stent is a wire mesh or implantable device that is permanently placed in the artery to keep it open and prevent it from narrowing.
What to Expect from Your PAD Treatment
Nationally Recognized Vascular Specialists
The American Endovascular affiliated physicians are proud to offer high-quality, compassionate PAD treatment and endovascular care for patients throughout New Jersey and New York. They perform a wide range of minimally invasive-image guided procedures to restore blood flow and return patients back to their podiatrist, primary care doctor, or wound care center for continued care.
Our team of board-certified vascular specialists is able to diagnose and treat peripheral artery disease and all manner of vascular conditions, including end-stage renal disease (ESRD) and venous insufficiency, in a safe and comfortable outpatient setting. Meet our affiliated physicians and learn more about their specialties, experience, and the world-class care they provide at American Endovascular.
What Our Patients Are Saying
Learn more about our patients’ experiences at American Endovascular.

Request an Appointment at your nearest American Endovascular affiliated center.
American Endovascular proudly serves men and women with peripheral artery disease in New York and New Jersey. Our vascular centers are equipped with a team of expert affiliated vascular specialists and cutting-edge endovascular technology and tools. Most of our outpatient centers are accredited by the Joint Commission and adhere to health code standards. When you visit American Endovascular, you’ll find private patient rooms, modern operating rooms, and separate recovery areas in an outpatient setting. Find your nearest vascular center in NY or NJ to request an appointment with one of our affiliated vascular specialists today.
Recent Blogs & Videos
Learn more about vascular health, prevention, and care for Peripheral Artery Disease.